
How Air Pollution Affects Health
Breathing polluted air makes people sick. When you breathe polluted air, the pollution passes through your lungs into your bloodstream. From there, it can reach your heart, brain, and other organs. Pollution can even pass through the placenta to affect a developing fetus. Pollution causes inflammation in your lungs and other body parts. Because of this, air pollution accounts for a large portion of deaths related to several major diseases.
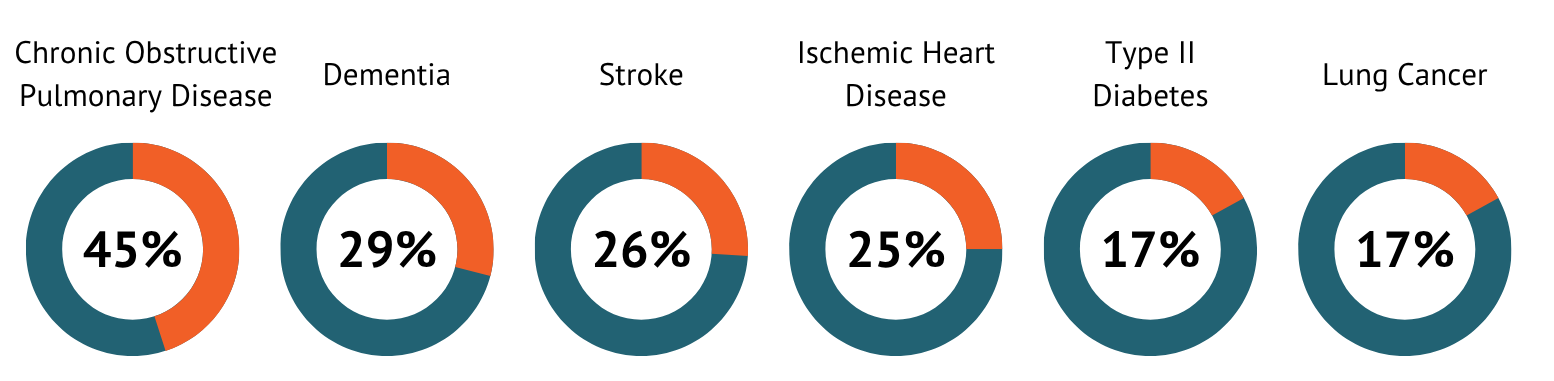
Air pollution does not affect everyone equally. People living in poorer regions suffer a higher disease burden, and most deaths occur in young children and older adults. This reflects differences in air pollution exposures as well as social, economic, and demographic factors that affect a person’s underlying health status, level of vulnerability, and access to medical care. Sometimes pollution causes health problems that are noticeable right away, but most problems build up gradually.
Total number of deaths attributable to total air pollution in 2023. Hover or tap to explore the data.










